ACLS Practice Questions ACLS PALS BLS
-
Quality CPR includes all of the following except?
- IV access should always be established above the diaphragm in the pregnant patient receiving CPR.
-
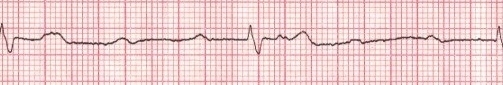
This patient would likely have an increase in pulse rate in response to atropine therapy.
-
An elderly patient’s family should be consulted, and give permission before the do not attempt to resuscitate (DNAR) prescription is written.
-
"Unstable" when referring to an arrhythmia means:
Want More Study Resources?
When you register for your exam, you get access to exclusive practice tests and case studies.
Get Access Now
Ready To Register For Your Exam?
ACLS
Included FREE:
- Instant Card and CE Certificate
- Case Study Library
- Online Review with Practice Questions
- Review and Retake of Exam
PALS
Included FREE:
- Instant Card and CE Certificate
- Case Study Library
- Online Review with Practice Questions
- Review and Retake of Exam
BUNDLE & SAVE
Get BLS Free When You Register for Both ACLS & PALS
- Instant Card and CE Certificate
- Case Study Library
- Online Review with Practice Questions
- Review and Retake of Exam