CASE STUDY NH1-1
You have been dispatched to a “person down” call and arrive on the scene within 2 minutes. Quality 1- person CPR is being administered by a trained witness/lay provider. A second lay rescuer arrives at the same time as you, and emergency ventilation is initiated at a rate of 100 compressions using a 30:2 ratio. You immediately place AED patches on the patient’s chest. CPR is interrupted while the AED is in the “analyze” mode. The unit advises you to shock the patient. Upon discharge of the AED, CPR is resumed; the patient is intubated and, IV access is established. A second shock is administered and CPR is resumed. There is no pulse. 1.0 mg of 1:10,000 (10 ml) of epinephrine is administered IV push and circulated for 2 minutes. A third shock is advised and delivered. A pulse is detected, and CPR is terminated. Assisted ventilation is continued while the patient is transported to the emergency department.
CASE STUDY NH1-2
While transporting a patient complaining of chest pain, you administer low-flow oxygen. You already have administered aspirin and nitroglycerin; completed a 12-lead ECG and have him on the monitor. Suddenly his eyes roll back, he stops breathing and is rapidly becoming blue. You glance at the monitor and see:
You immediately charge your biphasic defibrillator (automatically delivers 120 joules), apply conductive media and deliver the shock. The patient immediately begins to take deep breaths. You look over at the ECG monitor and see:
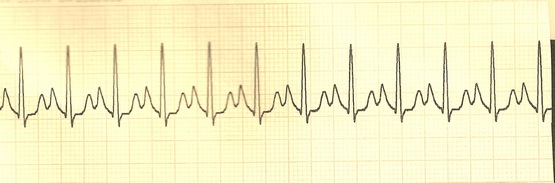
Over the next several minutes, the patient awakens and seems to be restabilizing, when suddenly the arrest reoccurs. This is what you see on the ECG monitor:
You again defibrillate him causing an immediate conversion. He is regaining consciousness, and the EMT trainee with you asks if he should get some epinephrine. Oxygen via nasal cannula is started, and you instruct him to get a syringe of lidocaine from the drug box. You administer 100 mg over a minute, and hang a 4 mg/minute continuous lidocaine infusion. You arrive at the hospital and transfer care to the awaiting cardiac team.